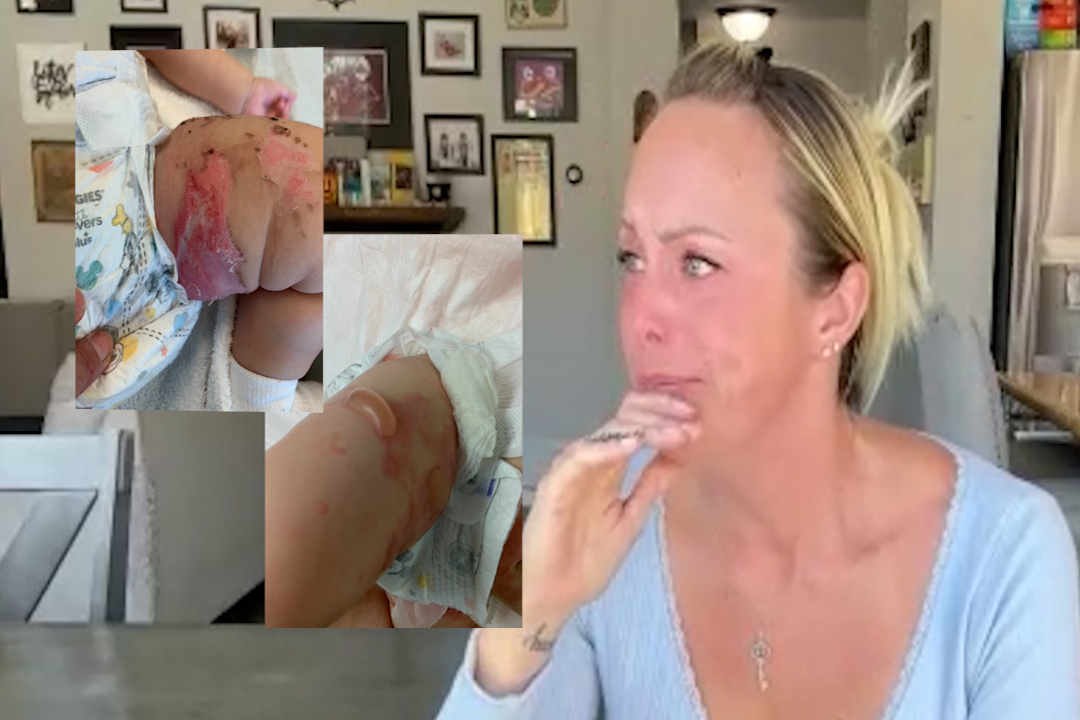
A California mother says an emergency room visit for her newborn turned into a shocking six-figure bill.
Jessica Farwell, from Antioch, told KGO-TV that in October 2022, a rice cooker fell off her kitchen counter and seriously burned her 6-month-old son, Brody.
“His skin instantly bubbled up,” she said. “I was afraid his face might start bubbling too.”
Jessica rushed Brody to a nearby hospital, where doctors gave him fentanyl through his nose to help with the pain. But the hospital didn’t have a burn unit or any ambulances to transfer him.
“They told me the wait for an ambulance would be seven hours,” she recalled.
Doctors decided it was medically necessary to send Brody to Shriners Children’s Hospital in Sacramento. Jessica offered to drive the 1 hour and 20 minutes herself, but the hospital refused, saying they had already called for a medical helicopter.
The 15-minute helicopter ride cost nearly $90,000. Jessica says she was told she wouldn’t get the bill because the hospital ordered the helicopter and she had insurance.
But after landing, she learned they also needed an ambulance to take them from the helipad to the hospital entrance — only 0.3 miles away. She says you could walk there faster, but the ambulance ride still cost $10,200.

Brody was treated for second-degree burns and released the next day. Months later, Jessica got the bill: $100,032. Insurance covered less than half of the helicopter bill and part of the ambulance bill, leaving her to pay $57,929.80 for the helicopter and $7,327 for the ambulance.
For three years, she says she made countless calls to the hospital, ambulance company, and insurance provider but got nowhere. Debt collectors started contacting her. Desperate, she reached out to KGO-TV for help.
After the station got involved, the entire bill was dropped. “They said, ‘It’s done, we will never bill you again,’” Jessica recalled. “It’s a miracle.”
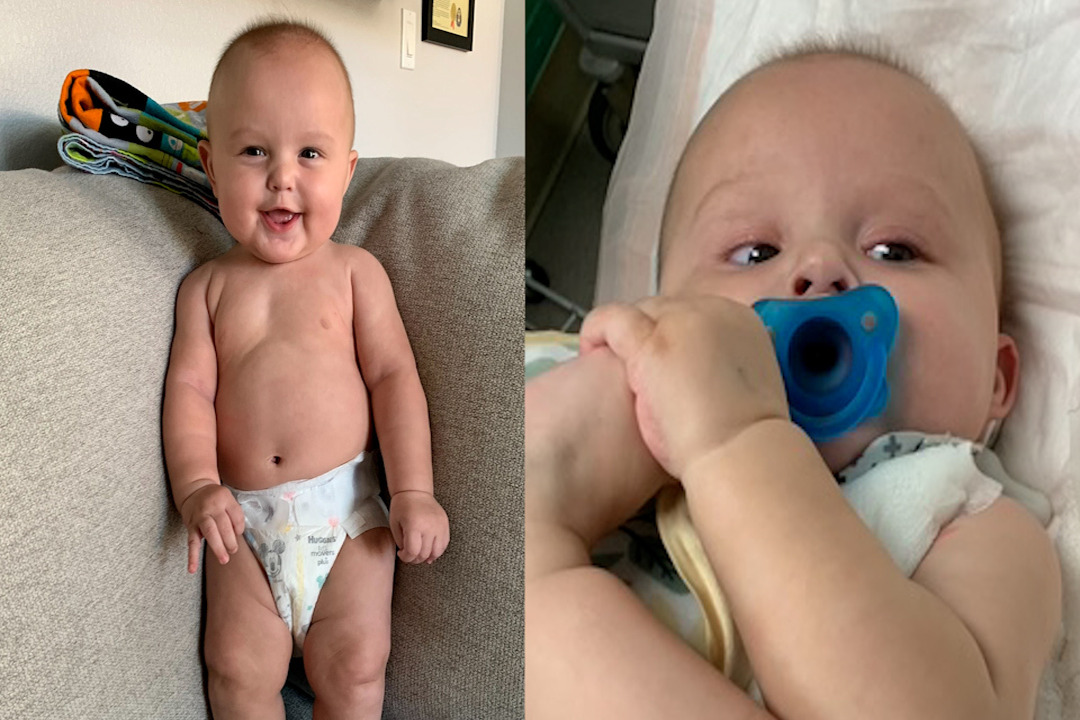
California passed a law in January 2024 that bans surprise bills for ground ambulance rides. But because Jessica’s case happened before the law, her ambulance bill wasn’t included.
The ambulance company said the problem was with the insurance company passing part of the bill to Jessica. They later agreed to take the partial payment from insurance and drop the rest.
Blue Cross Blue Shield, her insurer, said they could not comment on her specific case but remain committed to providing care according to each member’s plan.